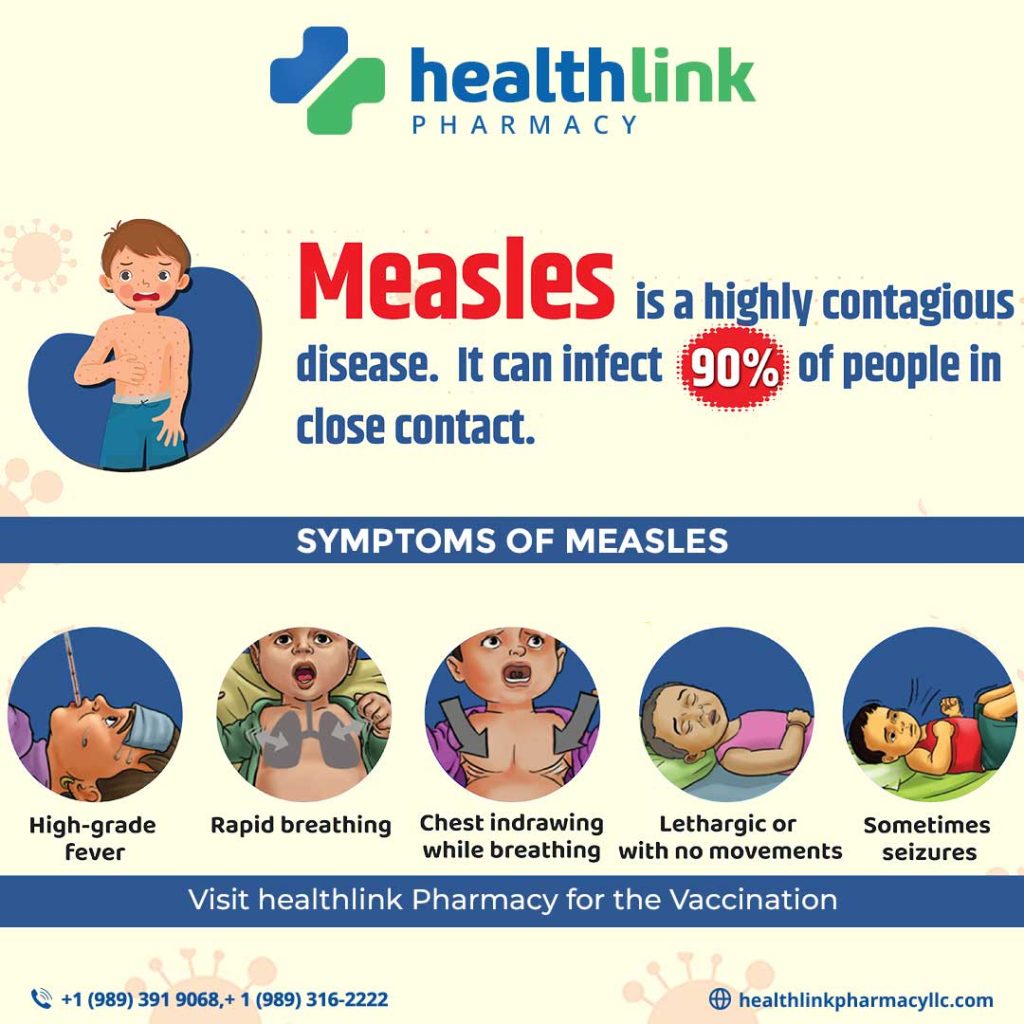
Measles outbreaks have become a growing public health concern, affecting communities worldwide. Despite being a preventable disease, measles cases have been rising in recent years, leading to significant health, economic, and social consequences.
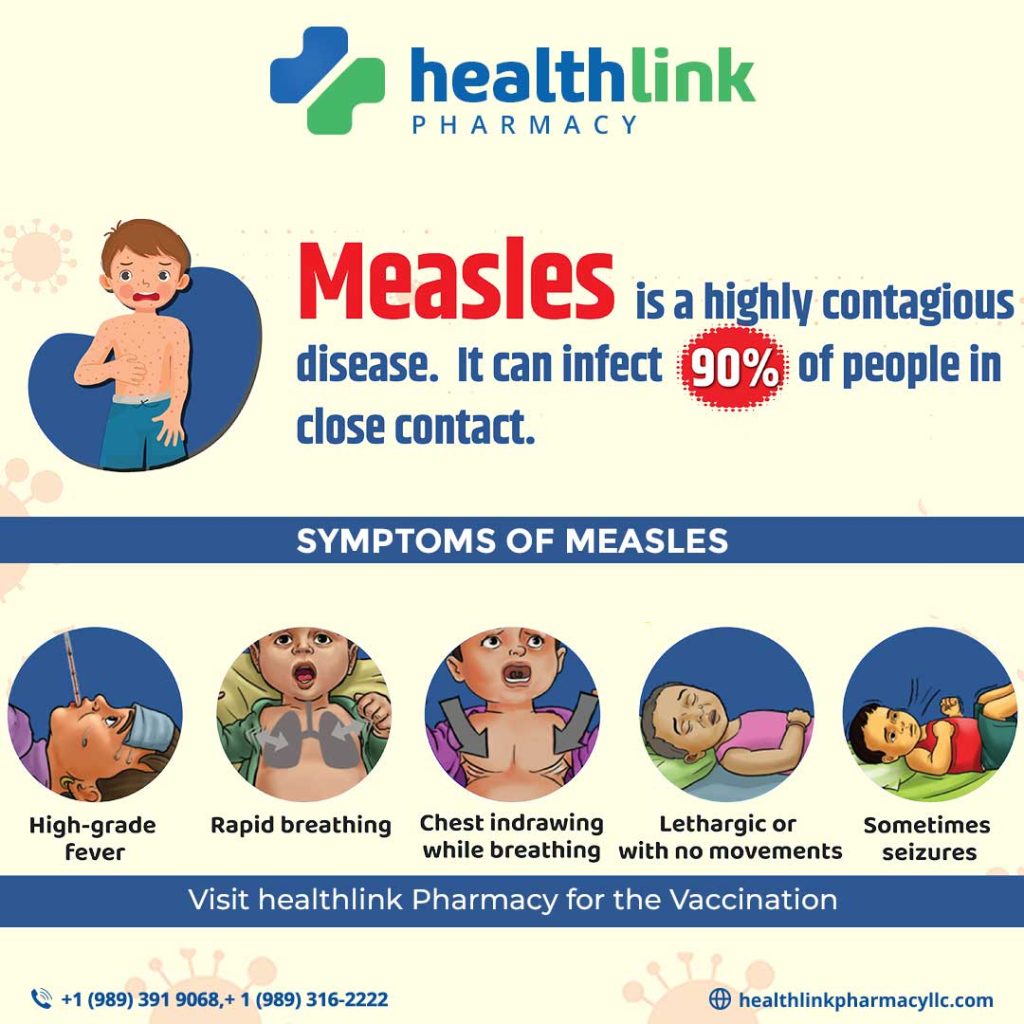
What is Measles?
Measles is a highly contagious viral disease caused by the Measles morbillivirus. It primarily affects children but can also infect adults. The disease presents with symptoms such as:
- High fever
- Cough
- Runny nose
- Red, watery eyes
- A characteristic red rash that spreads over the body
Measles can lead to severe complications, including pneumonia, encephalitis (brain swelling), and even death, especially in young children and those with weakened immune systems.
How Measles Spreads in Communities
Measles spreads through airborne respiratory droplets when an infected person coughs or sneezes. The virus can linger in the air and on surfaces for up to two hours, making it incredibly easy to contract. It is estimated that one infected person can spread measles to 90% of unvaccinated individuals in close contact.
Risk Factors for Transmission
- Low vaccination rates
- Crowded living conditions
- International travel
- Weakened immune systems
Recent Measles Outbreaks Around the World
In recent years, several countries have reported significant measles outbreaks. Notable cases include:
- United States (2019): The largest outbreak in decades, primarily due to vaccine hesitancy.
- Europe (2023): Countries like Romania and Ukraine saw thousands of cases.
- Africa: Continues to struggle with measles due to low immunization rates.
These outbreaks highlight the need for increased vaccination coverage and public awareness.
Why Are Measles Outbreaks Increasing?
Several factors contribute to the rise in measles cases, including:
- Declining vaccination rates due to misinformation and vaccine hesitancy.
- Increased international travel, spreading the virus to new regions.
- Weakened healthcare infrastructure in some areas.
The Role of Vaccination in Measles Prevention
The Measles, Mumps, and Rubella (MMR) vaccine is the most effective way to prevent measles. Two doses provide 97% immunity against the disease.
Herd Immunity: Why It Matters
When a high percentage of the population is vaccinated, it creates herd immunity, protecting those who cannot receive the vaccine, such as:
- Infants under 12 months
- People with severe allergies
- Immunocompromised individuals
Who is Most at Risk During an Outbreak?
While anyone can get measles, the most vulnerable groups include:
- Unvaccinated children
- Pregnant women
- Elderly individuals
- People with chronic illnesses
Complications and Long-Term Effects of Measles
Measles can lead to:
- Pneumonia, the leading cause of measles-related deaths
- Encephalitis, causing seizures or brain damage
- Subacute sclerosing panencephalitis (SSPE), a rare but fatal brain disorder that develops years after infection
Economic Impact of Measles Outbreaks
Measles outbreaks can have severe economic consequences, including:
- Increased healthcare costs due to hospitalizations
- Loss of productivity from missed work and school
- Government spending on outbreak control measures
Social Consequences of Measles Outbreaks
Measles outbreaks disrupt communities by:
- Forcing school closures
- Imposing travel restrictions
- Creating public fear and misinformation
How Schools and Workplaces Can Prevent Spread
- Ensuring vaccination requirements for students and employees
- Promoting good hygiene practices
- Quarantining infected individuals
The Ethical Debate Over Mandatory Vaccinations
Some argue that mandatory vaccinations infringe on personal freedoms, while others stress their necessity for public health. Countries with strict vaccination laws tend to have fewer outbreaks.
Frequently Asked Questions (FAQs)
How long does measles last?
The illness typically lasts two to three weeks, with symptoms improving after the first week of the rash.
Can vaccinated people still get measles?
While rare, breakthrough infections can occur, but they are usually mild.
Is measles deadly?
Yes, especially for young children and immunocompromised individuals. One in five unvaccinated individuals with measles requires hospitalization.
Why do some people refuse the measles vaccine?
Vaccine hesitancy is driven by misinformation, religious beliefs, and concerns about side effects, despite overwhelming scientific evidence supporting vaccine safety.
Can measles be eradicated?
Theoretically, yes. High vaccination rates and global cooperation could eliminate measles.
Conclusion
Measles outbreaks pose a significant threat to public health, but they are preventable through vaccination and community awareness. Governments, healthcare providers, and individuals must work together to ensure high immunization rates and combat misinformation to protect future generations.